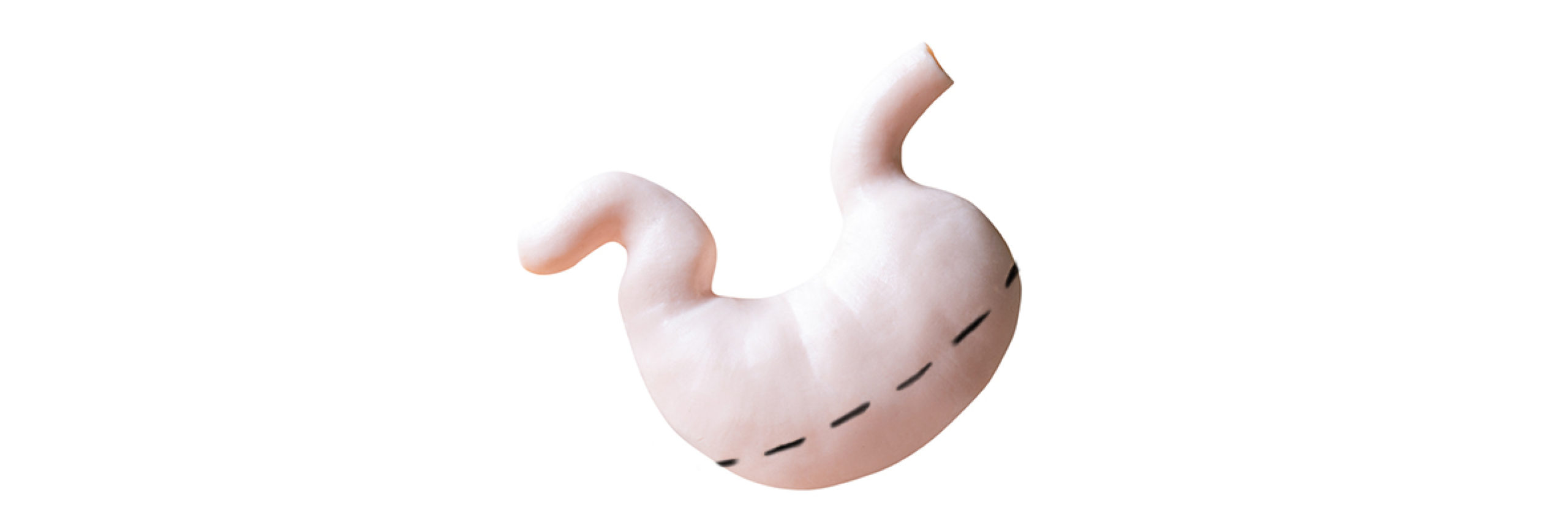
Gastrectomy
Criteria for suitable candidate
- 32 – 45 BMI / 15 – 45 years old
- A patient with 50+ BMI may be acceptable for the operation if a patient is younger than 50 years old and has no serious conditions that affect the use of anesthetic.
Surgical Procedure
Gastrectomy is a procedure of permanently removing your stomach, partially or entirely. It’s often used with stomach cancer patients and obesity. The surgeon will divide and seal any blood vessels supplying the part of the stomach to be removed. The stomach is then surgically stapled and sealed using a calibration guide tube to measure the size of the stomach tube left behind, removing around four-fifths of the stomach permanently. This is known as a restrictive operation, which means it restricts the amount of food / drink that your smaller stomach will be able to hold after surgery. Your stomach can usually hold up to 2,000ml but this reduces to less than 150 ml.
* 5 NIGHTS
1 - 2 HOURS
GENERAL ANAESTHESIA
Pre Operative Care
 Before your surgery, please inform the surgeon of any allergies, all medical conditions, and any medication that you are taking (both prescription and non-prescription medications).
Before your surgery, please inform the surgeon of any allergies, all medical conditions, and any medication that you are taking (both prescription and non-prescription medications).  Patients with hypertension must inform the surgeon prior to the surgery to eliminate the chance of postoperative bleeding, and should avoid any medication containing, Aspirin or Brufen, for 2 weeks prior to the surgery.
Patients with hypertension must inform the surgeon prior to the surgery to eliminate the chance of postoperative bleeding, and should avoid any medication containing, Aspirin or Brufen, for 2 weeks prior to the surgery. Smoking is also prohibited for 2 weeks prior to the surgery, as smoking can affect your reaction to the anaesthetic and slow down the healing process.
Smoking is also prohibited for 2 weeks prior to the surgery, as smoking can affect your reaction to the anaesthetic and slow down the healing process. 
Post Operative Care
1. Please inform your surgeon of your medical condition and any medication/s that you are taking (both prescription and non-prescription), any allergies, all medical conditions (such as bronchial asthma, diabetes, hypertension, blood clotting abnormalities, etc.) and provide us the updated test result 1-2 months before the surgery date.
2. Stop taking aspirin, medications containing ibuprofen, all vitamins and herbs for at least 1 week prior to surgery to eliminate the chance of post-operative bleeding. Please consult your attending physician before stopping anticoagulant medication.
3. Stop smoking for at least 1-2 weeks prior to surgery as this will prolong your healing process from vasoconstriction.
4. No food and any liquid in take for at least 8 hours prior to consultation & surgery.
5. Absolutely no alcoholic beverages for at least 48 hours prior to appointment.
6. Make sure you do not wear any jewelries, piercing, make up and nail polish to surgery.
7. You should shower the morning of your surgery, wash your hair and do not apply any perfume, lotion, powder, cream or deodorant.
Post Operative Care and Recovery Expectations
On the first or second day, you will be asked to start drinking water. Once this is confirmed to be normal, you will eventually start your diet plan. Until this test is completed, you will often have IV fluids (drip) to make sure you have enough fluid in your body and therefore do not get dehydrated. You will have 1 follow-up appointment after discharge.
Eating and drinking after surgery
You will not have anything to eat or drink until you can start drinking water. During this time, you will receive fluids to hydrate you through a drip. You may get very dry mouth; the nurses will offer you mouth washes and you will be able to gargle as long as you do not swallow anything.
Then you will be able to start drinking water 1,200ml, very slowly at first. At meal times, you will also be able to start having a soft diet.
Over the next few weeks, you will be able to have pureed food, then to solid one. Your meals will be much smaller and you may have to stop drinking with meals due to your small stomach.
You will need to make significant lifestyle changes after surgery to lose weight and keep it off. You’ll probably need to take vitamins or other supplements for life. You will also have to, and be able to, increase the amount of physical activities you do.
You will not be discharged until you are managing to eat and drink successfully.
How much weight will I lose and what effects will it have?
Sleeve gastrectomy surgery can help reduce 30-50% of the original weight. This can improve symptoms like fatigue, shortness of breath and improve quality of life such as your energy levels, ability to walk and exercise and potentially reduce pain in weight bearing joints and the back. In addition, several medical conditions can improve resulting in reduced need for medication. These includes:
– Type 2 diabetes
– High blood pressure
– Sleep apnea (interrupted breathing during sleep)
– High cholesterol
– Polycystic ovaries
Risks and Complications
The major operative risk is leakage of staple line (usually 1% in all center). But with our surgeon, Dr. Thakoon, more than 400 cases of our patients have experienced 0% leakage. The surgeon usually do stiches cover the staple line with omentum to reduce the leakage risk. In case there is any leakage, it usually happens in 1 week after surgery and a patient will have to stay longer in the hospital, up to 2-4 weeks.
Immediate and short term complications:
– Wound infection
– Bleeding
Longer term complications:
– Stomach ulcers
– Strictures
– Adhesions
– Nutritional deficiencies after surgery
– Less predictable drug and alcohol absorption
– Depression and maladaptive eating (uncommon)
– Weight gain and recurrence of obesity related illness
What must I do to ensure my operation will work long-term?
Any weight loss surgery can fail to help you lose weight if vital lifestyle changes are not made before and after surgery, or end up with disappointing weight regain if these changes are not continued. Only you can make these changes. This is why we prepare you for surgery over at least 6 months to ensure you are making the correct changes in diet and exercise to ensure it will succeed.
– A diet consisting of regular 3 low sugar meals per day
– Avoidance of drinking liquids with meals
– Avoidance of snacks like crisps and sweets or sugary juices/drinks
– Consider other ways to improve your mood or relax instead of relying on food